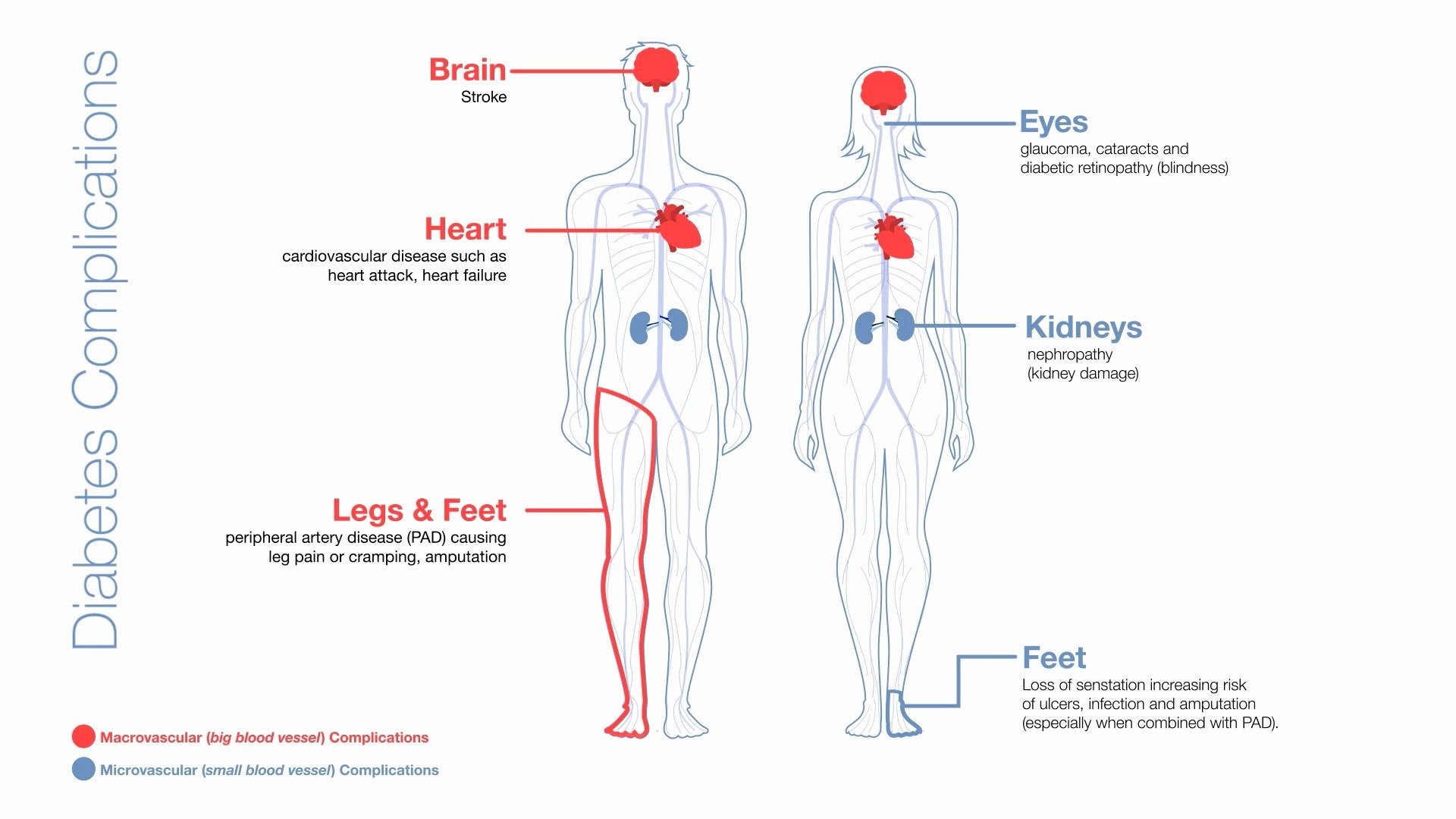
People with diabetes are often reminded to have regular check-ups for their eyes, kidneys and feet to detect any changes that may result from consistently high blood glucose levels, but rarely think about diabetes and sexual health when first diagnosed. High blood glucose levels not only cause macrovascular complications (damage to large blood vessels, including the heart), they also cause microvascular complications (damage to small blood vessels). Microvascular complications can create problems with the eyes (called retinopathy), nerves (called neuropathy) and kidneys (called nephropathy).
It’s not entirely clear how diabetes causes complications. Some theories suggest that the direct damage is caused by excess glucose in the blood, while others point to indirect mechanisms, such as molecules in the body that have been altered by high blood glucose levels or by tissue inflammation.
The truth of the matter is that these damages to small blood vessels are not limited to the eyes, kidneys or feet; they can also affect other areas of the body. When the small blood vessels and nerves in the genital areas are affected, sexual problems can arise. Microvascular complications and sexual problems can worsen more quickly if blood glucose, blood pressure or cholesterol levels are poorly controlled, or with tobacco use.
What sexual problems can occur in men with diabetes, and how are they treated?
Erectile dysfunction: The biggest cause of sexual issues for men is nerve and blood vessel damage in the genital area, which disrupts blood flow, causing erectile dysfunction. Erectile dysfunction is defined as a consistent inability to have an erection firm enough for sexual intercourse. The condition includes the total inability to have an erection or the inability to sustain an erection. Erectile dysfunction is known to occur in more than one-half of men who have had diabetes for 10 years or more.
Treatments for erectile dysfunction include the following:
- Oral medications called PDE-5 inhibitors (available in Canada under the trade names Viagra®, Cialis® and Levitra®) work by increasing the flow of blood into the penis so that when a man is sexually stimulated, he can get an erection. Although these medications can be used safely in most men with diabetes, including some elderly men, they are not safe for men with certain heart conditions or men who take nitrates (medications that are used to treat angina), due to the increased risk of blood pressure dropping too low, and too quickly.
- Injection of a medication called alprostadil (the trade name is Caverject®). This medication is injected into the blood-filled space of the penis to achieve erection before intercourse.
- Intraurethral suppository, using a small alprostadil pellet, is inserted into the urethra to help stimulate blood flow.
- Mechanical methods: a vacuum device can create an erection by pulling blood into the penis using a pump, with a constriction ring placed at the base to maintain the erection.
- Surgical methods: There are inflatable and malleable (bendable) implants, surgically placed into the penis to facilitate erections. These are typically a last resort due to their invasive nature.
Other sexual problems in men with diabetes include the following:
Retrograde ejaculation is a condition whereby semen passes backwards into the bladder instead of through the tip of the penis. In men with diabetes, retrograde ejaculation can result from damage to the sphincter muscle at the neck of the bladder. Raised blood glucose levels can damage the sphincter muscle and the nerves that control it, meaning that the sphincter doesn’t close properly and allows semen into the bladder.
Retrograde ejaculation is not harmful, and only needs to be treated if you are trying to father a child. Medications that help tighten bladder neck muscles can be prescribed. Controlling blood glucose levels can help, but couples who are trying to conceive may need to use assisted fertilization procedures.
Low libido, which is caused by inadequate production of the male sex hormone, testosterone. Men with type 2 diabetes are at risk of testosterone deficiency, particularly if they are also overweight.
Losing weight, controlling blood glucose levels and getting regular exercise can help prevent and treat testosterone deficiency in men with diabetes. Testosterone replacement therapy may be used in some cases.
Mental health support can help address underlying issues like depression that may impact libido. Many Canadian provinces provide coverage for psychological therapy.
What sexual problems can occur in women with diabetes, and how are they managed?
Diabetes-related nerve damage can cause vaginal dryness that makes intercourse uncomfortable. Nerve damage can also lead to loss of sensation in the genital area, making orgasm difficult or impossible to achieve.
Lack of lubrication and painful sex: Dryness of the vagina, due to a lack of lubrication or slow lubrication, can lead to painful intercourse. It is thought that nerve and blood vessel damage in diabetes contributes to this effect. The problem is easily remedied by using a water-soluble personal lubricant, which should provide relief from discomfort during sex. These are widely available in Canadian pharmacies and on-line. Estrogen therapy and vaginal dilators are other treatments to help manage this issue.
Reduced arousal and difficulty achieving orgasm: This can be caused by diabetic neuropathy and poor blood circulation which reduces genital sensation. Treatments include topical creams, pelvic floor therapy and improved blood sugar control.
Infections: Women who suffer from poor blood glucose control are more susceptible to vaginal yeast infections, because the yeasts flourish in high sugar environments. Thrush can be treated with antifungal cream or a vaginal suppository.
Loss of desire: Losing interest in sex is not the sole domain of women with diabetes. Decreased sexual desire can be due to many factors, but one that does relate to women with diabetes is widely fluctuating blood glucose levels. Poor control of blood glucose can lead to tiredness and a lack of interest in sex. Bringing blood glucose levels under control may help restore desire.
Can diabetes-related sexual problems be prevented?
Both men and women with diabetes can lower their risk of sexual problems if they:
- Maintain blood glucose levels within target ranges
- Maintain blood pressure and cholesterol levels in the ranges recommended by their healthcare providers
- Adopt a healthy lifestyle which includes physical activity, healthy eating, quitting smoking and limiting alcohol intake.
- Maintain a healthy weight
- Have regular health checkups to help identify issues early
- Get mental health and stress management support
In Canada, diabetes and sexual health are closely connected, as high blood sugar levels can influence numerous body functions essential for healthy intimacy. By recognizing the specific challenges for men and women, understanding available treatments in Canada, and adopting preventive measures, individuals with diabetes can improve their sexual health and overall quality of life. With the right lifestyle modifications, open communication, and support from healthcare providers, Canadians with diabetes can lead fulfilling intimate lives.