If you have diabetes, it is important to know what the A1C test is, why it is important, and how the diabetes team uses the A1C in managing your diabetes.
What is an A1C blood test?
The A1C test is a common blood test that measures the amount of glucose in the blood. The A1C blood test goes by many other names, including A1C, HbA1C, glycated hemoglobin, glycosylated hemoglobin or hemoglobin A1C. Hemoglobin is a protein found in the red blood cells that carries oxygen to the cells. Glucose attaches to hemoglobin in your blood cells, and the A1C test measures the amount of hemoglobin with attached glucose.
The test results reflect your average blood sugar over the past 2-3 months. As your red blood cells have a lifespan of around 3 months, this is why the test gives us an average of what has been going on in your blood for the past few months.
The higher your A1C level, the greater your risk of developing diabetes, and the poorer your blood sugar control if you already have diabetes.
What A1C number is used to diagnose diabetes?
When an A1C is equal to or greater than 6.0%, this is diagnosed as pre-diabetes. When A1C is equal to or greater than 6.5% this is a diagnosis of diabetes. A test should always be repeated on a different day to be sure of the diagnosis.
| A1C | Percentage |
| Normal | Below 6.0% |
| Prediabetes | 6.0-6.4 % |
| Diabetes | 6.5% or greater |
How does the A1C relate to average blood sugar?
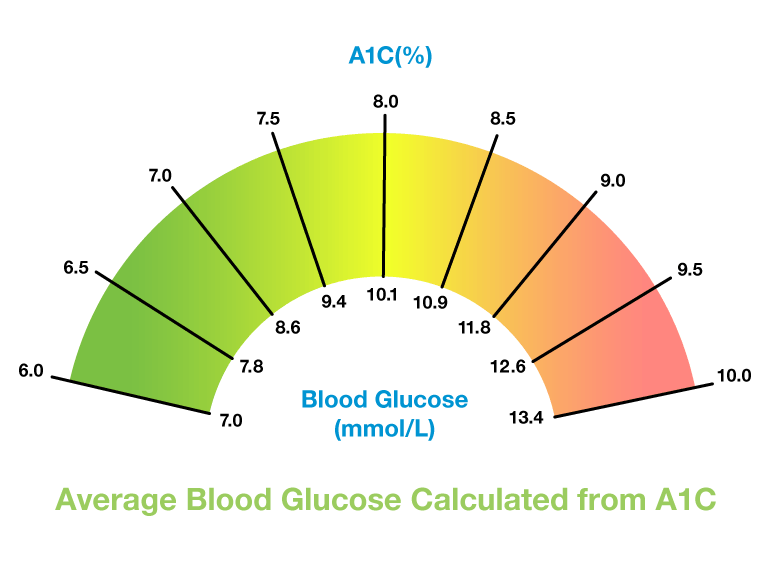
A1C is measured as a percentage, (for example: an A1C of 7%). This does not correspond to an average blood sugar of 7 mmol/L however (the number a person would get from their glucometer). There is a formula that converts the A1C to an average blood sugar. The table below shows an A1C % and the corresponding average blood sugar level in mmol/L, which is the measurement used in Canada.
| A1C (%) | Average Blood Sugar (mMol/L) |
| 6 | 7.0 |
| 6.5 | 7.8 |
| 7 | 8.6 |
| 7.5 | 9.4 |
| 8 | 10.1 |
| 8.5 | 10.9 |
| 9 | 11.8 |
| 9.5 | 12.6 |
| 10 | 13.4 |
Why is the A1C test done?
The A1C blood test is one of the primary methods of diagnosing prediabetes, type 1 diabetes, and type 2 diabetes.
After diagnosis, the test is used to monitor your response to treatment, how well your diabetes is being managed, and if any changes need to be made to medications or your treatment plan. A1C is a better reflection of your diabetes management as it tells a story of your blood sugar over a period of time, in comparison to the blood sugar levels you measure at home, which are just a snapshot at a specific point in time.
Your doctor will likely repeat the A1C test a few months after diagnosis, and at least 2-4 times a year thereafter depending on what type of diabetes you have, what medications you are taking, if you use insulin, if there are any changes to your treatment plan, and how well your diabetes is managed.
What is the target A1C for a person with diabetes?
For most people, the A1C target should be 7% or lower (this is usually attained by having pre-meal blood sugars of 4-7 mmol/L and post-meal blood sugars of 5-10 mmol/L).
If a person is very elderly or frail, a young child, or someone at risk of having low blood sugars, then the A1C target can be a bit higher (8% or 8.5 %). It is important to individualize your A1C target with your diabetes team.
What does it mean when the A1C and the blood sugars don’t match?
Sometimes a person’s A1C doesn’t seem to match their blood sugar readings at home. If this is the case, it usually means that they are not measuring their blood sugars often enough to see the fluctuation in blood sugars. For example, an A1C might be elevated (for example 9%) but the person gets very normal readings in the morning (7 mmol/L). However, they may not be testing later in the day when their readings might be very high (12 mmol/L).
Why does a person need to test their blood sugars if they can get an A1C?
The A1C is only an “average” blood sugar reading. This can be made up of highs and lows. If someone is on a treatment that doesn’t cause lows (for example, only metformin), then they don’t need to do blood tests as often and the A1C is fairly representative of their average blood sugar. However, blood testing will give specific information on the ‘pattern’ of their blood sugars, showing when they are high and low, and what lifestyle factors such as food and exercise cause them to be higher or lower.
If a person is on insulin, self-monitoring their blood sugars is extremely important because it can give moment-to-moment information on how to adjust insulin. If a person’s blood sugars are out of range, then testing gives information on what time of day to target therapy. For instance, if the morning numbers are higher, they may need nighttime insulin. Or if the morning numbers are at target but blood sugar is high after supper, they may need more medication at suppertime.
Is the A1C ever inaccurate?
The accuracy and effectiveness of A1C tests may be limited in certain cases. If you experience heavy or chronic bleeding, your A1C test may be falsely low. If you have iron deficiency anemia, B12 deficiency, alcoholism or kidney failure, your A1C test may be falsely high. These situations (among others) would make the A1C less representative of the average blood sugar, and would be less useful for people with diabetes.